🧠 Why Reimbursement Matters Right Now
Online therapy isn’t just a pandemic trend—it’s the new normal. Millions now prefer video or phone-based sessions for mental health care, and insurers are finally catching up. But whether you’re fully insured, out-of-network, or paying cash, knowing your online therapy insurance reimbursement options can save you hundreds—sometimes thousands—every year.
🔍 Why 2025 Is a Pivotal Year for Teletherapy Coverage
- 🏥 Medicare now permanently covers behavioral telehealth—even audio-only calls.
- 📅 Telehealth flexibilities remain extended through September 30, 2025, across all states.
- 🧾 44 states + DC require private insurers to reimburse teletherapy like in-person care, thanks to expanding payment parity laws.
💬 Case Example (Johnson Box)
“I didn’t think I could get reimbursed for therapy over Zoom,” says Maya, a freelance designer. “But once I got a superbill and submitted it, I got 70% back. I saved over $900 last year.”
If you’re paying out-of-pocket, chances are your health plan—or even the IRS—will give you some of that money back. All it takes is knowing how to choose the right payment path and submit the proper documentation.
📆 What These Deadlines Mean for You

Understanding these milestones can maximize your reimbursement chances and help you plan smarter:
- Medicare Coverage (Jan 2025): Seniors and those on disability can now get reimbursed for therapy sessions—even by phone. No video? No problem.
- State Parity Laws (Ongoing): If you live in one of 44 states (plus D.C.), your insurer must treat telehealth the same as in-person care. That includes mental health!
- Flexibility Expiration (Sept 30, 2025): Some temporary rules allowing audio-only or out-of-state therapists may expire. Don’t delay filing your claims.
- Parity Final Rule (Jan 1, 2026): This upcoming federal rule strengthens your appeal rights. If your claim is denied, you’ll soon have new legal tools to push back.
🧾 Pro Tip: Mark these dates in your calendar. If your sessions fall within these protected windows, you’re more likely to get reimbursed or win an appeal.
💳 Three Ways to Pay & Get Paid Back
Most online therapy users fall into one of three reimbursement paths. Whether you’re insured, paying cash, or stuck in a deductible limbo, there’s a path that can help you save—or even get money back.
🔁 Overview Table
| Path | Best For… | What You’ll Do | Typical Out-of-Pocket |
| 🧾 In-Network Billing | Your plan partners with the therapy platform | Enter your insurance member ID; pay only your copay | $0–$40 per visit |
| 📤 Out-of-Network + Superbill | Your therapist/platform doesn’t bill your plan directly | Pay upfront → get superbill → file your own claim | 20–50% of session fee (after claim) |
| 💸 Cash-Pay + Tax Tools | No insurance or high deductible | Use discount plans, HSA/FSA, or deduct costs on taxes | $60–$120/week (tax-deductible) |
🔍 Which Path Are You On? (Decision Help)
Quick Tip: Ask your therapist or platform: “Do you bill my insurance directly, or will I need to submit a superbill myself?”
If they say yes → You’re in-network.
If they say no → You’ll need to pay first and submit (Path 2).
If you don’t have insurance → Go straight to Path 3 for cost-saving tools.
🧾 Real-Life Scenarios
- Nina, 33 (In-Network): Uses Talkspace with Aetna. Enters her member ID at checkout. Pays just a $25 copay per session.
- Carlos, 41 (Out-of-Network): Sees an independent therapist. Pays $120 per visit, gets a superbill, submits it to Cigna, and gets $72 reimbursed after his deductible.
- Jules, 29 (Cash-Pay): No mental health coverage. Uses Online-Therapy.com, pays $95/week via HSA card, and deducts the rest on taxes.
🧠 Pro Tip: Once Your Deductible Is Met…
Even with out-of-network providers, many plans reimburse 50–80% of the insurer’s “allowed amount.” Keep tracking your expenses—it could flip the math in your favor later in the year.

🧾 How Online Therapy Gets Coded (And Why It Matters)To receive reimbursement, your therapy session must be accurately coded. These codes are like the “language” your insurer speaks. If any part is missing or wrong, your claim could be delayed or denied.
Let’s break down what your therapist needs to include on a superbill or claim for online therapy insurance reimbursement in 2025:
🧠 1. CPT Codes: What Service Was Provided?
CPT stands for Current Procedural Terminology. These codes explain what type of therapy was done, and how long it lasted.
✅ Key 2025 CPT Codes for Online Therapy:
| Code | Format | What It Means |
| 98000–98007 | Video/Hybrid | Standard online therapy (video or video + digital tools) |
| 98008–98015 | Audio-only | Phone-based therapy (replaces 99441–99443) |
| 90833, 90836 | Add-on codes | Pair with medical evaluations or extended time |
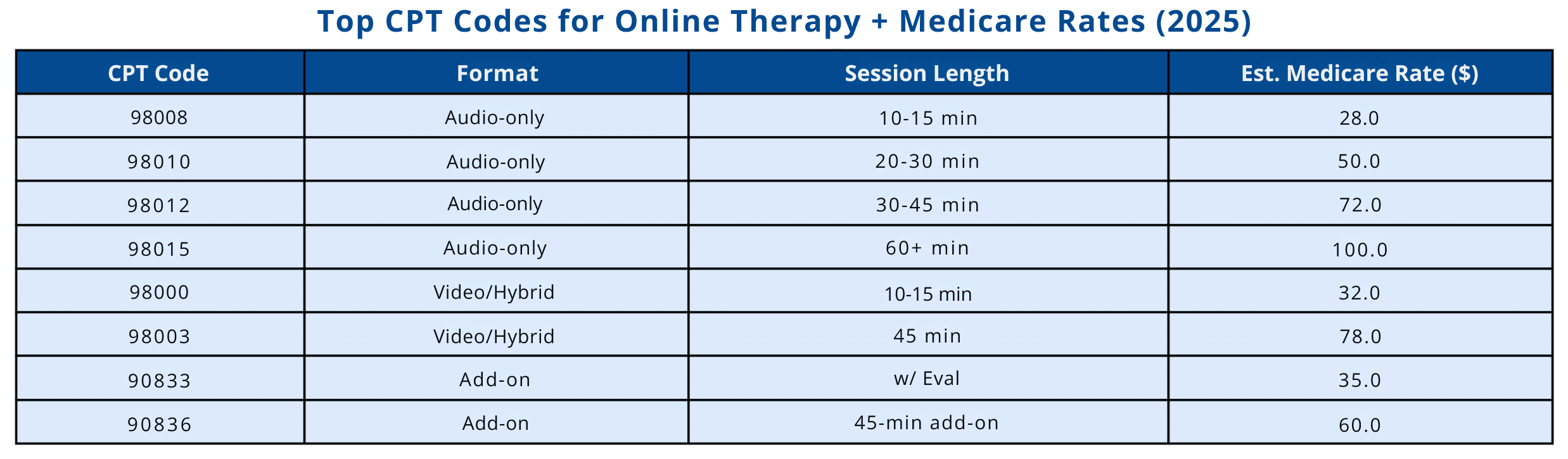
📌 CPT 98008 is typically used for 10–15 min audio-only therapy. CPT 98015 may be used for sessions lasting 60 minutes or more.
💻 2. Modifier 95: The Virtual Visit Tag
This modifier tells the insurer that the session was conducted via telehealth. Even if the CPT code is correct, missing Modifier 95 can result in a rejected claim.
Example:
CPT 98012-95 (indicates a 30-minute phone session conducted remotely)
📍 3. Place of Service (POS) Codes: Where the Session Took Place
POS codes tell the insurer where the client was during the session:
| Code | Meaning |
| POS 10 | Patient was at home (most common in 2025) |
| POS 02 | Patient was remote, but not at home (e.g., at a clinic or work) |
🚫 Some insurers default to POS 02—you may need to request that billing update this to POS 10 for home-based therapy.
🔍 4. Diagnosis Code (ICD-10): Why Therapy Was Medically Necessary
Every claim must include an ICD-10 diagnosis code—typically assigned from the DSM-5 (e.g., F41.1 for Generalized Anxiety Disorder). This establishes “medical necessity” in the insurer’s eyes.
✅ Reimbursement Coding Checklist
✔ CPT code from 98000–98015
✔ Modifier 95 (for telehealth)
✔ POS 10 (if client was at home)
✔ Valid ICD-10 diagnosis (from DSM-5)
✔ Provider’s NPI and license credentials (included on superbill)
“Top CPT Codes for Online Therapy + Medicare Rates (2025)” Table
⚠️ Common Mistake Watchlist
| Mistake | Fix |
| CPT code correct, but Modifier 95 missing | Ask the provider to refile with the modifier |
| POS code set to 02 instead of 10 | Request resubmission with the correct location |
| Diagnosis too vague or missing | Ensure ICD-10 code from the therapist matches your session type |
🧾 Path 1 – Use Insurance Directly
Good news: Many online therapy platforms now bill insurance directly. If your provider is “in-network” with your health plan, you can often just enter your insurance info at checkout and pay only your copay.
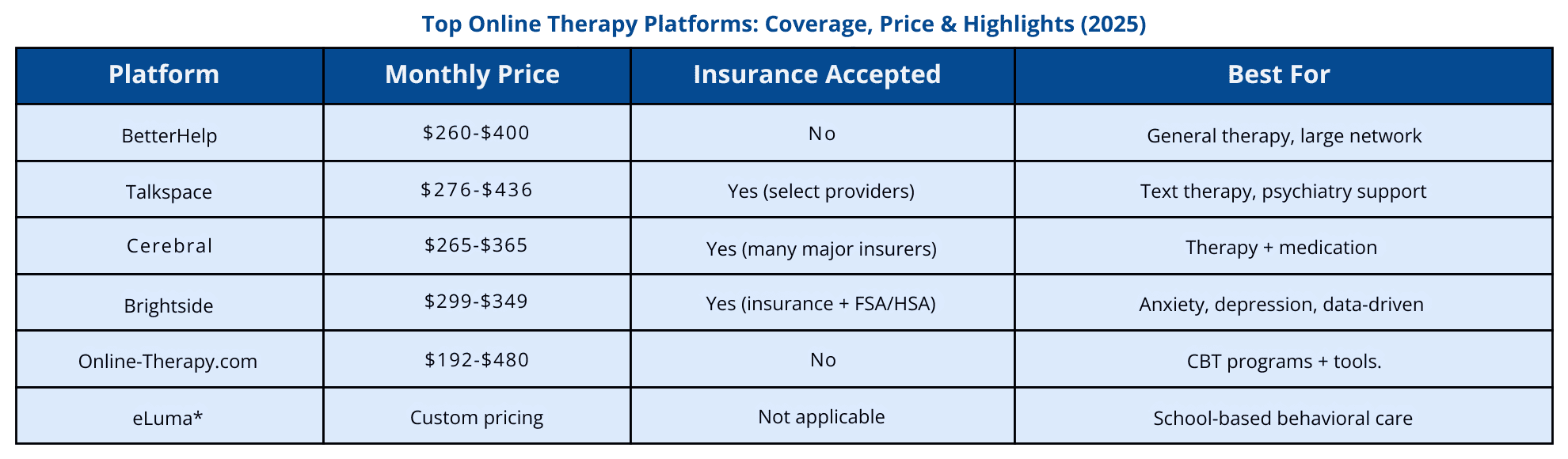
✅ Top Platforms That Accept Insurance
| Platform | Major Insurers Accepted | Instant Coverage Check? | Notes |
| Brightside | Aetna, Cigna, BCBS, Medicare | ✔ | Also provides superbills for OON claims |
| Talkspace | Anthem, Optum, UHC, EAPs | ✔ | Covers ~131M insured lives |
| Cerebral | Most commercial PPOs | ✔ | Separate therapy-only plan; FSA/HSA friendly |
| BetterHelp / Eluma / Online-Therapy.com | ❌ | — | No direct billing – use Path 2 instead |
🗣️ 5-Step Script: How to Confirm Coverage Before You Book
Before you schedule your first appointment, call your insurer using the number on the back of your insurance card. Ask the following:
- “Do I have telehealth mental health coverage?”
- “Is [Therapy Platform] in-network under my plan?”
- “What’s my copay, deductible, and coverage for behavioral health?”
- “Do I need prior authorization or referrals for telehealth visits?”
- “Can I use my FSA/HSA for any remaining balance?”
✍️ Pro Tip: Keep a notepad or spreadsheet with the date, representative’s name, and what they told you. It’ll help if there’s a billing issue later.
🔎 What to Expect After Booking
- ✅ Insurance accepted: You’ll see your copay at checkout (usually $0–$40).
- 📄 Explanation of Benefits (EOB): Your insurer sends this summary after the session. Check that it matches what you were charged.
💬 Real Example:
Alex, 38, uses Talkspace + Optum.
He signs up, enters his member ID, and is matched with a licensed therapist. At checkout, he pays just $20 per session, and Talkspace bills Optum directly.
🧠 Quick Reminder:
If your platform says, “We don’t bill insurance,” don’t panic. You’re not out of options—just switch to Path 2: Superbill Submission.
🧾 Path 2 – Pay First, Claim Later
If your therapist or platform doesn’t accept your insurance directly, you can still get reimbursed—you just need a superbill and a bit of follow-through.
✅ What’s a Superbill?
A superbill is a detailed receipt that your therapist provides, which includes all the essential information your insurer needs to process a reimbursement:
Required Elements on a Superbill |
| Provider’s full name & NPI number |
| Session dates & CPT codes |
| Diagnosis code (ICD-10) |
| Total fee per session |
| Place of service (usually POS 10) |
| Modifier 95 for telehealth |
💡 Tip: Always double-check that the superbill includes Modifier 95 and POS 10 to indicate a home-based telehealth session—otherwise, claims often get denied.
📝 How to File a Reimbursement Claim (DIY)
Most insurers follow a similar process:
- Get the superbill from your therapist after your session(s).
- Log in to your health plan’s member portal or download a CMS-1500 form (standard claim form).
- Upload or mail the form along with:
- The superbill
- Proof of payment (credit card/bank statement)
- Track the status via your insurer’s portal or by calling member services.
- Expect reimbursement in 2–6 weeks (via check or direct deposit).
📂 Pro Tip: Always keep digital or paper copies of what you submit. If there’s a denial, this will help you file an appeal faster.
🤖 Automation Help: Use Reimbursify
If doing it yourself feels intimidating, tools like Reimbursify can:
- Scan & submit your superbill
- Auto-fill claim forms
- Track payout timelines
- Send alerts if your claim is delayed
💡 First claim? Try filing manually to understand the process, and then decide if automation is worth the small fee.
💸 No Insurance? Lower Costs Up Front
If you’re paying entirely out of pocket, don’t worry, there are still smart ways to lower your therapy costs and potentially recoup some value through tax tools.
🔹 1. Try Low-Cost Online Therapy Platforms
These platforms offer affordable, flat-rate plans—sometimes with financial aid or sliding scales:
| Platform | Weekly Price | Session Types | Notable Features |
| Online-Therapy.com | $65–$125/week | Messaging, video | CBT-based tools, worksheets, financial aid |
| Brightside (no insurance) | $95+/month | Video, messaging | Anxiety & depression focus |
| Cerebral (non-insurance plan) | $95–$365/month | Video, medication mgmt | Therapy + psychiatric care |
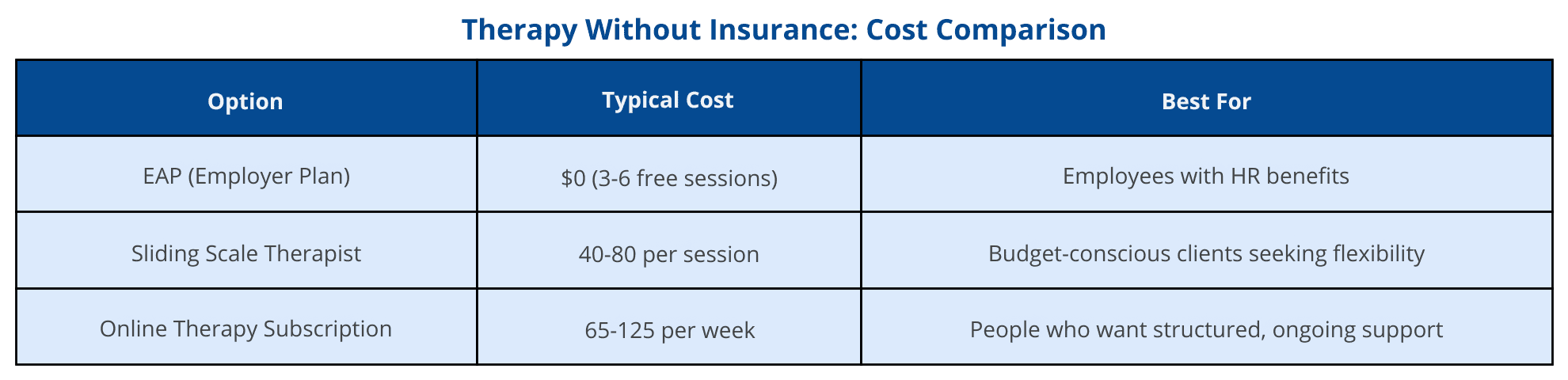
🔹 2. Explore Sliding Scale or EAP Options
- Sliding Scale Therapists: Try free matching quizzes on therapy directories like Open Path or Zencare to find licensed therapists starting at $40/session.
- EAPs (Employee Assistance Programs): Many employers offer 3–6 free sessions—even if you don’t have insurance through them.
💡 Pro Tip: EAP sessions are confidential and often underused—check your HR portal!
🔹 3. Use Tax-Advantaged Accounts (or Deduct Your Expenses)
You may be able to save hundreds at tax time by paying with:
- HSA (Health Savings Account) – tax-free for qualified therapy expenses.
- FSA (Flexible Spending Account) – use-it-or-lose-it style tax-free funds.
- Itemized Deductions – if therapy + other medical costs exceed 7.5% of your AGI, you may be able to write them off.
📎 Acceptable documentation includes:
- Therapist invoices or superbills
- HSA/FSA card statements
- Bank/credit card receipts
📅 2025 Coding & Policy Changes to Watch
Understanding changes to codes and coverage rules can help you stay one step ahead—and successfully challenge unfair denials.
🧠 Why Knowing These Codes Matters
When it comes to getting reimbursed, knowing the correct CPT codes (Current Procedural Terminology) isn’t just for therapists—it can save you money and prevent claim denials.
Here’s why:
- ✅ Insurance companies require precise codes to identify the type of therapy you received. An incorrect code—or a missing modifier—can lead to automatic denial.
- 💡 Patients with out-of-network benefits often submit claims themselves. Knowing what to look for on your superbill helps you verify accuracy before you file.
- 🛡️ If a claim is denied, knowing the right code allows you to spot the issue and request a corrected claim or file an appeal confidently.
- 🧾 These codes also help you maximize tax deductions for therapy if you’re itemizing medical expenses.
In short, understanding these codes transforms you from a passive patient into an empowered healthcare consumer.
📞 New CPT Codes for Audio-Only Therapy
As of 2025, the CPT 98008–98015 family has officially replaced older codes like 99441–99443 for phone-based therapy.
| Code Range | Description | Session Length |
| 98008–98010 | Audio-only therapy (brief) | 10–25 minutes |
| 98011–98013 | Audio-only therapy (standard) | 30–45 minutes |
| 98014–98015 | Audio-only therapy (extended) | 50+ minutes |
➡️ Why it matters: Submitting claims with outdated codes (like 99441) may result in automatic denial. Ask your provider to confirm they are using the current CPT code set.
⚖️ Mental Health Parity Final Rule (Effective Jan 1, 2026)
This landmark rule requires that mental health benefits are treated with equal generosity as medical benefits—especially for:
- Deductibles
- Copays
- Session limits
- Prior authorization
📌 Use it in appeals: If your therapy claim is denied for reasons like “not medically necessary” or “not covered,” cite the 2026 Mental Health Parity Rule as part of your appeal documentation.
💡 Pro Tip: Save a link or PDF of the final rule so you can attach it during appeals or denials—it boosts credibility.

🚫 Common Denials & How to Fix Them
Even with the right codes, claims can still get rejected. Here are the most common denial reasons for online therapy reimbursement—and exactly how to fix them:
| ❌ Denial Reason | 🧭 Why It Happens | 🔧 Quick Fix |
| Missing Modifier 95 | The telehealth tag was left off the CPT code. | Ask your therapist to refile with Modifier 95. |
| Wrong Place of Service | Insurer defaulted to POS 02 instead of POS 10. | Request billing to update claim with POS 10. |
| “Not Medically Necessary” | Diagnosis code was missing or too vague. | Include full DSM-5 diagnosis and treatment plan. |
📝 Pro Tips for Smoother Appeals
- Keep a call log: Document every insurer conversation—note the date, name, and what was discussed.
- Attach proof: Include your therapist’s treatment plan, superbill, and a short letter explaining medical necessity.
- Use templates: Save time with a pre-written appeal letter—download our editable version here.
🧠 Appeals work: Most insurers have a formal appeal process—and many patients win if documentation is clear and complete.

❓ FAQs: Online Therapy Insurance Reimbursement
Q1: Does Medicare cover Talkspace or other online platforms?
A: Sometimes. Medicare may cover Talkspace only if:
- The therapist is credentialed with Medicare
- The session is conducted via live video (not chat-based)
Always confirm with the platform and Medicare before booking.
Q2: Can I get reimbursed for chat-based or text therapy?
A: Rarely. Most insurance plans require real-time interaction (video or phone). However, some plans may:
- Let chat sessions count toward your deductible
- Reimburse part of a hybrid plan if video is included
Q3: What CPT code should I use for a 15-minute therapy check-in?
A: Use:
- CPT 98016 – For brief telehealth check-ins (2025 code)
- CPT 99421 – If your insurer still uses the older E-visit series
➡️ Tip: Always confirm code compatibility with your provider and plan.
Q4: Can couples or family therapy be reimbursed if done online?
A: Sometimes. Use:
- CPT 90847 – Family/couples therapy with patient present
- Add Modifier 95 to show it was telehealth
Check your plan’s policy—some require prior approval for family sessions.
Q5: Can I use HSA or FSA funds for online therapy?
A: Yes! Therapy is a qualified medical expense under both Health Savings Accounts (HSA) and Flexible Spending Accounts (FSA). Just save:
- Invoices or superbills
- Payment records for documentation
✅ Key Takeaways
✔️ Check your coverage
→ 44 states now require insurers to reimburse telehealth at the same rate as in-person therapy. Even audio-only therapy may qualify.
✔️ Don’t have insurance?
→ Use low-cost online platforms, HSA/FSA funds, or itemize your therapy expenses. You may still recoup up to 80% of costs through tax strategies.
✔️ Use the correct CPT codes
→ For 2025, use CPT codes 98000–98015 for online sessions and always include Modifier 95 and POS 10. Outdated codes = denied claims.
✔️ Denied a claim? Appeal it.
→ Most denials are fixable. Common issues include missing modifiers or vague diagnoses. Attach full documentation and cite the 2026 Mental Health Parity Rule.
✔️ Get matched to the right provider
→ Take our Provider Match Quiz to compare platforms like Brightside, Talkspace, Cerebral, and Online-Therapy.com—all in one place.
🧭 Suggested Next Step:
💬 Not sure which online therapy platform fits your coverage, budget, or goals?
🎯 Take our 2-minute Provider Match Quiz and get instant personalized results.
👉 Start the Quiz Now →











